The use of virtual environments to help train surgical procedures is now well established and there are many examples of both research systems and commercial products that support a wide variety of surgical specialisms. Our own work has included developing training tools for neurosurgery. For example, a tablet-based solution demonstrated that it is not necessarily a requirement to use expensive hardware and software to produce an effective training tool for the ventricular catheterisation (ventriculostomy) procedure, the insertion of an external ventricular drain. In a validation study, statistically significant changes in performance of selecting the burr hole entry point, the trajectory length and duration metrics for the group that used the tablet training tool (called VCath), together with a good indicator of improved normalized jerk (representing the speed and smoothness of arm motion), all suggest that there was a higher-level cognitive benefit to using the training tool, compared to the control group that only received conventional training.
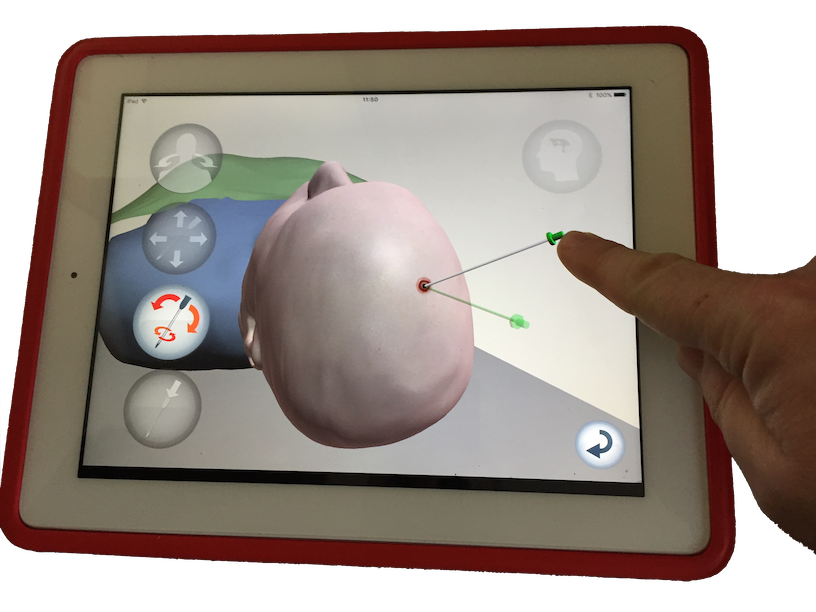
We subsequently created a higher fidelity version of VCath to investigate whether the use of stereoscopy - so that the virtual patient in the training tool is rendered in three dimensions (3D), in life-size - could further improve the training of a ventriculostomy procedure.
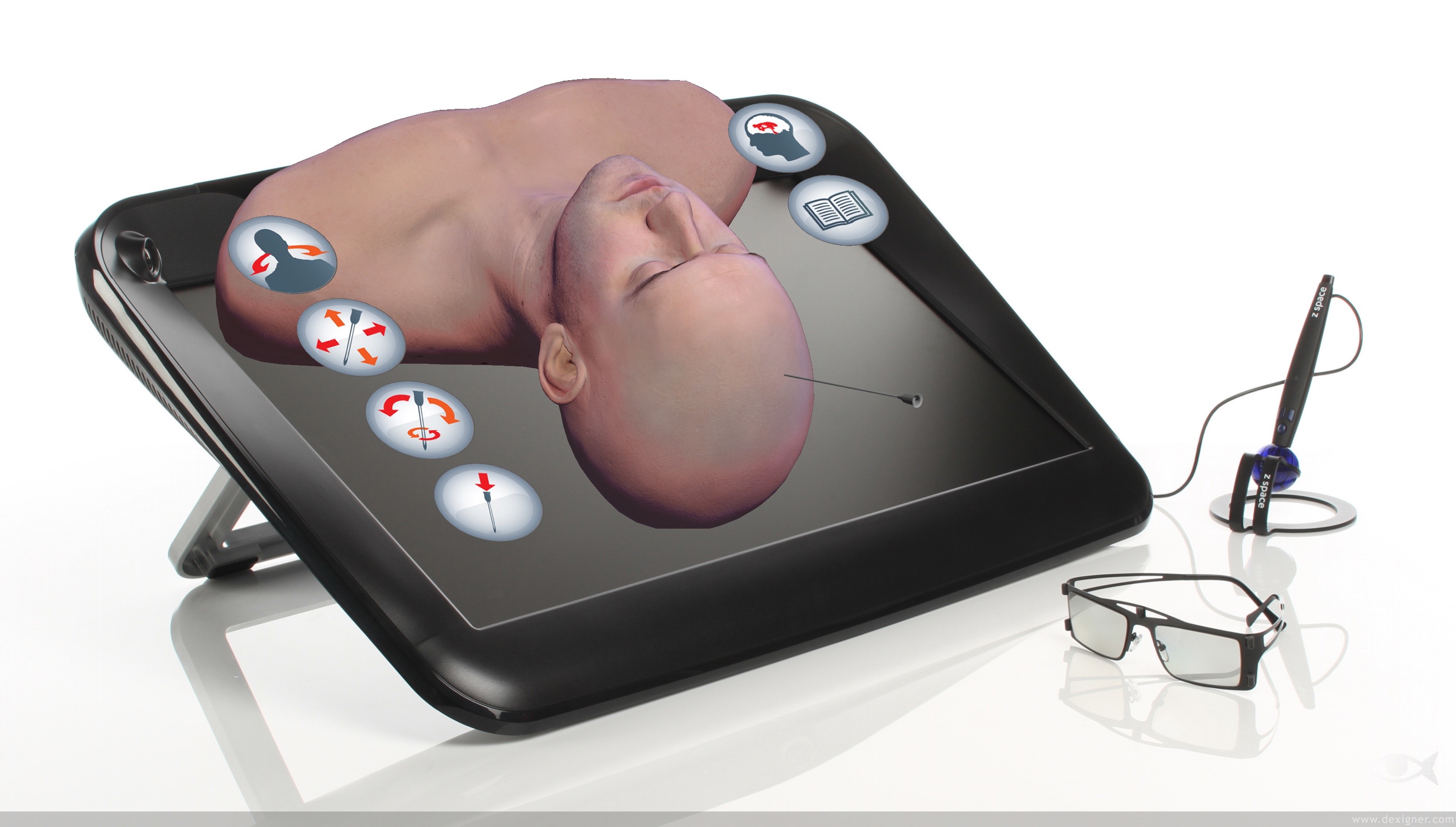
However, a subsequent validation study showed that there was no strong benefit from the use of stereoscopy for training this task (see references for more details). The educational benefit of our tablet simulator appears to be as good as, if not better, than our high fidelity version in improving procedure skill. The crucial factor for performing a successful cannulation is to have a 3D appreciation of what you are trying to do. Commonly this is achieved by dividing the procedure into a series of formal steps (although some surgeons will do this informally, subconsciously). The metrics we have used are aimed at capturing these steps. These steps are qualitatively different, and sequential, and as such cannot really be thought of as being more or less important than one another, or summing to a weighted-average performance. The practical methodology for performing the task in patients involves measuring from anatomical landmarks for the burr hole placement then lining up the catheter along two anatomical vectors. These can all be achieved as two-dimensional tasks and so the addition of stereoscopy to the simulation may not provide any added benefit in developing the skills needed for this procedure. The target ventricles are not normally visible and so in any case once the entry point has been selected and insertion begins, stereoscopy will cease to have any effect on the outcome. With training simulators predominantly aimed towards inexperienced junior doctors, the use of low fidelity models issues a compelling argument towards the use of widely accessible inexpensive provision to supplement their formal education.
Collaborators: Leeds General Infirmary, Bangor University, Salford Royal NHS Foundation Trust